
CM-Path hosted a workshop on sample quality in biobanking and promoting best practice
Research Engagement Manager, Emma Lawrence reports back on the workshop.
Although I had used human samples in research in the past I had never given much thought to what makes a ‘good quality sample’. This week I attended the NCRI CM-Path initiative’s “Biobanking best practices workshop” to find out about their new quality improvement tool. I found out that there’s a lot more to quality than I had thought.
Starting with the donor
We kicked off by talking about issues surrounding patient engagement and consent. Catherine Blewett of the HRA opened the day with a talk about the future of consent. She summarised the results of a recent IPSOS MORI study on public opinion. I was surprised to find out that there was very limited knowledge about research and human tissue initially. Once the value of biomedical research was explained, however, there was a strong feeling that samples should be used. The public were also reassured by data security and came to understand the important role of commercial companies in biomedical research. The main findings were that the public want the samples to be used providing they are asked, informed and that the maximum benefit is achieved.
Catherine explained that currently there is variable consent completion rates depending on who is taking the consent. She’s therefore working with Prof Andy Hall to develop optimised consent models with the aim of to maximising research outputs. This includes developing: Generic information sheets, Routine consent forms, Electronic recording keeping, and ensuring patients are kept updated. The idea is to optimise the process of when consent is taken, and by whom!
Maggie Wilcox from ICPV spoke about why Biobanking is important from the patient perspective. I really enjoyed Benjamin Johnson’s overview of how informed consent is obtained at the university of Southampton; a lot of energy is put into making patients feel included and appreciated. For example, when patients self check-in to clinic a prompt about research is included as a pre warning. Copious amounts of chocolate is also used in Southampton! All in all I Iearnt a lot about “quality” ways of engaging with patients and talking about consent.
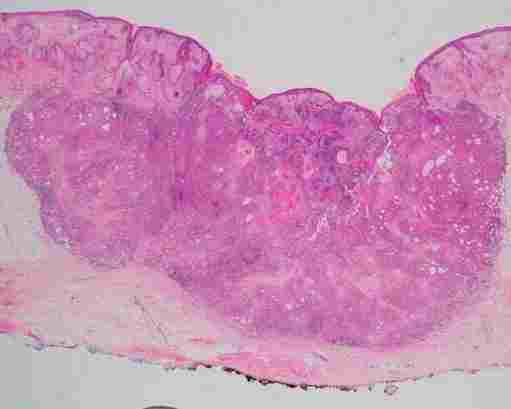
Cutaneous SCC (H&E stain)
Getting Surgical
I really enjoyed learning more about what goes on in theatre at the “sharp” end of biobanking. Dr Emma King provided us with insights from a head and neck cancer surgeon. She spoke passionately about engaging with surgeons and surgical teams in the process. Emma’s team uses varied ways of reminding surgeons to take samples straight away such as writing notes on old X-ray lights! She argued that taking the sample as soon as possible guarantees the best quality. Emma also seemed to have achieved the impossible by negotiating with health and safety to allow liquid nitrogen in surgical theatres!
In the following discussion the question of how to “bribe” surgeons into cooperation was raised. Emma made the great point that surgeons should not get on papers just for providing samples. I think patient advocate Maggie Wilcox hit the nail on the head when she argued that it’s the patient’s choice, not the surgeons. I think the take home from this session was to think creatively when working in teams.
Talking Pathology
I know that pathology is a vital part of biobanking so it was great to hear the perspectives of imminent pathologists Prof Gareth Thomas and Prof Louise Jones. Gareth reminded us that pathologists are there primarily to make a diagnosis, which is the priority before research. He advised that good communication with pathologists is essential for the collection process to work smoothly. Louise further tackled the challenges of being a pathologist by experimenting with vacuum packing samples. She showed that there was no difference in DNA and RNA yield, mitosis count or tumour grade in breast cancer samples when vacuum packed compared to refrigerated. This seems like an exciting prospect for biobanking, although further work on gene expression profiles does needs to be done. Watch this space!
Time to self-asses
In the afternoon Harriet Foden of NCRI launched the new CM-Path quality improvement tool. Harriet described how the tool was developed, using work by the Confederation of Cancer Biobanks (CCB) and consulting with different stakeholders. Importantly the tool is free and accessible for everyone and builds on areas on already covered by the HTA and Healthcare improvement Scotland. The tool is a confidential way of Biobanks improving their standards and will be useful training for new starters. You can access it here, and CM-Path are keen for you feedback on the tool.
The workshop was a great chance to catch up with colleagues in the biobanking and pathology community. I learnt that public involvement, communication and team work are vital parts of running a biobank.

